
COVID-19 Vaccination Management For Employers: Webinar Recap
The Alliance and Business Health Care Group (BHCG) hosted a webinar with several content experts to discuss employee communication strategies, policy and procedures, and other employer considerations regarding COVID-19 vaccination. This is a recap of the virtual event. Click here to view the full recording. Click to skip to the Employer Resources section.
How important is workforce vaccination for employers?
The Wisconsin Department of Public Health kicked off the event by explaining a large fraction of population needs to be vaccinated to achieve herd immunity, and that employers play a critical role in vaccination communication.
They produced an anonymous survey that had 4,451 employer-respondents answer questions about their roles in vaccination, the importance of vaccination, and barriers to vaccination. Below are some of those results:
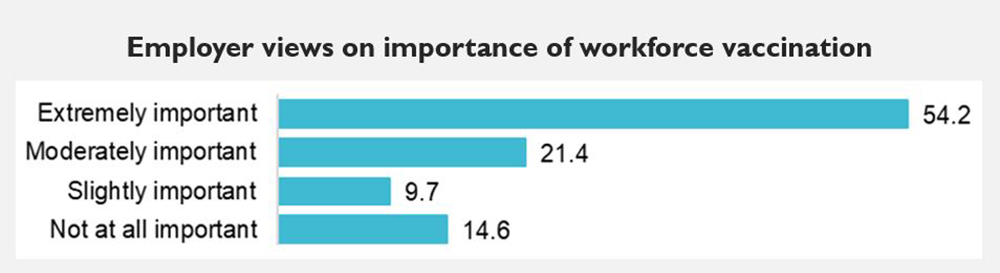
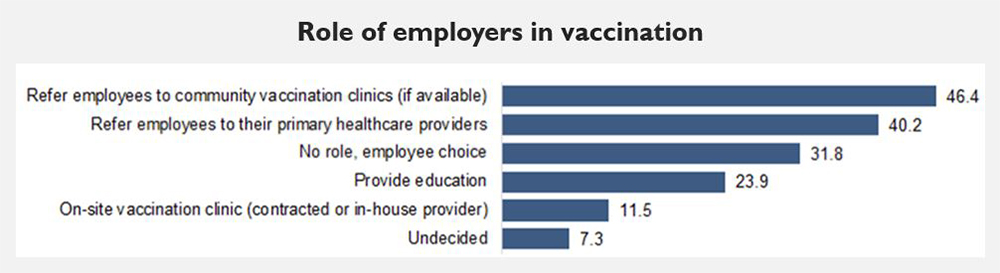
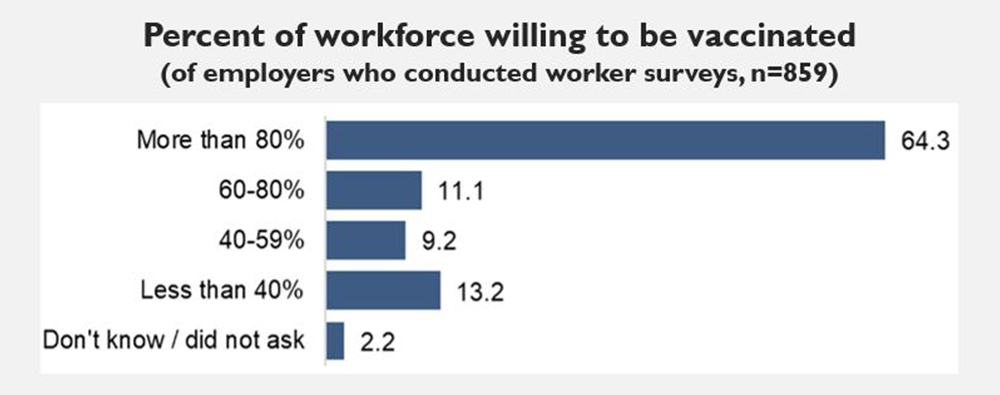
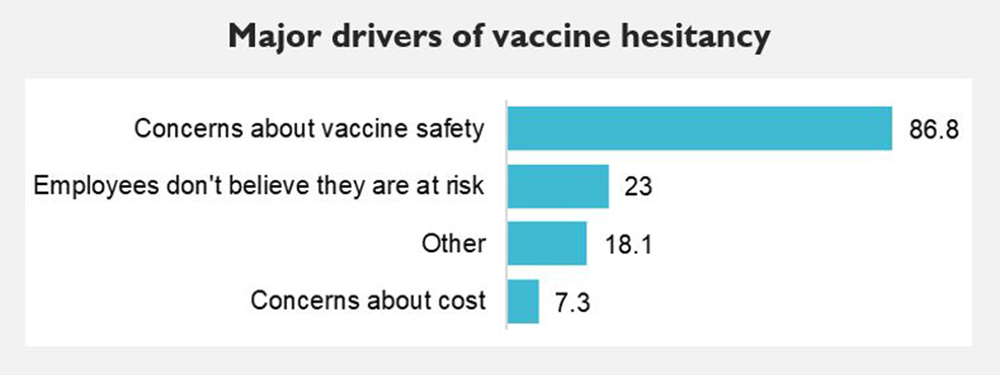
According to these results, three out of every four employers surveyed believes that:
- They play some role in getting employees vaccinated.
- Workforce vaccination is at least moderately important.
- At least 60% of their workforce is willing to get vaccinated.
How can employers encourage vaccination among employees?
Per the Wisconsin DHS, employers can help encourage vaccination using three methods: offering education, reducing barriers, and providing incentives.
- Educate: Utilize trusted messengers (health care providers, DHS/CDC, company management), address vaccine efficacy and safety concerns, use multiple communication channels (flyers, meetings, company intranet,) and account for differential reading levels and languages spoken.
- Reduce Barriers: Support paid leave to allow employees to get vaccinated, support paid leave for employees with side effects, host employer-sponsored vaccine clinics.
- Offer Incentives: Studies show that offering a financial incentive to get vaccinated can reduce unvaccinated workers by as much as 30%.
Practical Vaccination Considerations for Employers
As previously mentioned, educating employees about the safety and efficacy of vaccine side effects is important to break down misinformation; symptoms are usually minor and short-lived, quickly subsiding after two days. However, there are some practical concerns employers should consider.
Fever, fatigue, chills, and muscle aches are possible, uncommon symptoms, and on occasion, may result in lost work time. Ideally, employees should stay home with a fever and only return to work once it has been resolved.
It’s possible for an employee to contract COVID-19 the day they are scheduled to be vaccinated. If an employee reports symptoms such as cough, shortness of breath, sore throat, and loss of taste/smell, it’s very unlikely those symptoms would be caused by the vaccine. Employees with these symptoms should be tested for COVID-19 and follow the CDC’s guidelines for possible virus infection.
It should be noted, per CDC guidelines, that quarantine after COVID-19 exposure is not required after an employee is fully vaccinated (both doses,) within 3 months of their last dose, and have no symptoms. Employers should still use physical barriers, masks, and other meaningful safety measures to keep all their workers healthy, as it will take quite some time for herd immunity to take effect, if at all.
If employers take an active role in getting their workforce vaccinated, they may consider staggering their vaccination schedules to account for any absences due to side effects. (For example, they may vaccinate 1st shift on a Monday, and 2nd shift on Thursday.) Staggering is probably more important after the 2nd dose because more symptoms are usually more severe after the second dose.
A challenge with staggering vaccination schedules comes down to the logistical administrative burden and using a two-dose series of vaccinations could delay your workforce’s overall vaccination rate. To reduce the possibility of lost-work time due to side effects, employers might consider scheduling their employee vaccinations on a Friday.
Employer options for approaching vaccination in the workplace
Lindsey Davis, Partner at Quarles and Brady, and a member of the firm’s Labor & Employment Practice Group, outlined three possible roadmaps employers can follow in regard to vaccination programs.
Compulsory vaccination programs: This method requires the vaccine and best protects the workplace and community’s health.
- Reduces costs of absences, lost productivity, and long-run medical care.
- Better allows employers to open and stay open.
- Defends against civil liability
- Protects against enforcement action
Downsides:
- Significant administrative undertaking.
- Potential employer liability related to vaccine
- Navigating distrust of the vaccine in the workplace
- Need to develop an exemption process and consider accommodations
- Disciplining and/or terminating employees for noncompliance
Industries that might consider this option would have high levels of contact between employees and customers, frequent and close-proximity contact between employees, and businesses that depend on a high level of comfort for patronizing customers. Those industries could include: Healthcare, Dining and Hospitality, Customer-Serving Businesses, Educational Institutions and Daycares, and the Travel industry.
Employers with a union presence or who have less “high-risk” work environments would not consider a compulsory vaccine program.
Should an employer choose this vaccination program, they will also need to determine:
- How to track compliance and identify what proof of vaccination is required
- Make a plan to process exemption requests (both medical and religious)
- Strategize how to build employee buy-in (education, incentives, etc.) and plan for conflict diffusion.
- Assess how to minimize (and if possible, eliminate) vaccination costs
- Anticipate employee time-off requests due to the time necessary to receive the vaccine or adverse vaccination side effects
- Consider any potential discriminatory impact of a narrowly tailored vaccination requirement. (For example, if vaccines are required only for employees who cannot work remotely)
- Create and communicate a vaccination policy
Employer-Encouraged vaccination programs: This method is often the most popular choice for employers.
Positives:
- Administrative ease
- Higher employee morale and retention rates
- Less liability risk for discrimination claims
Downsides:
- Lower compliance than a compulsory program
- Widespread uncertainty and disinformation surrounding vaccines
- Cost of incentives
- Potential that incentives are deemed coercive and/or discriminatory.
Employers who might consider would operate in workplaces that do not require close contact, or one that can accommodate remote work, but one in which that arrangement is winding down.
Should an employer choose this vaccination program, they would also need to determine:
- How to track compliance and identify those who have received the vaccine
- Take a thoughtful approach to continued PPE and distancing requirements
- Consider incentives (paid time off, vaccination bonus, reimbursement for transit and childcare costs, etc.
- Consider practical implications for employees who choose against vaccination (reminding employees they may be required to quarantine without paid time off, etc.)
- Create and communicate a vaccination policy
Voluntary vaccination programs: This program does not encourage or incentivize vaccination and negates some legal risks, but brings about different ones.
Positives:
- Avoids certain legal risks (but opens the door for other risks, noted below)
- Low administrative costs
- Less practical difficulties (obtaining proof of vaccination, forms, processes, etc.)
Downsides:
- Other legal risks – potential for a case to be made the employer is not creating a safe work environment (OSHA, Tort, or Workers’ Compensation claims)
- Harmful business implications by not creating safe space for customers
- Diminished employee morale and retention from employees that want vaccine
This strategy is more practical for remote workforces: Finance, Marketing, Consulting, Customer Service, etc. Employers who might not consider a voluntary vaccination program include: Healthcare, Education, Emergency Response, Public Transportation, and Food Retail Services.
Should an employer choose this vaccination program, they would also need to distribute educational materials and create and communicate a vaccination policy.
Best Practices for employers and the vaccines:
There are a few options when it comes to vaccination policy for employers, and the best one depends upon an employer’s industry, the nature of their operations, and the overall size of their workplace. No matter what stance an employer takes on vaccination policy, here’s a summary of general rules they should follow when implementing a workplace strategy:
- Lead by example: having your C-suite get vaccinated before everyone else may be beneficial.
- Educate and empower your employees using reliable information from trusted educational resources: CDC, WHO, FDA, and DHS
- Be transparent with your workforce on policy and be prepared to answer questions
- Have a plan and policy regarding COVID-19 vaccination, and depending on your size, consider creating a COVID-19 task force that meets on a regular basis
- Maintain safety precautions (washing hands, wearing masks, and social distancing); mitigation strategies are still critical during vaccine rollout








