
Has your family faced these choices due to high costs of health care?
A college education or health care bills? Health insurance to cover future needs or health care for what ails you right now? Medicine or food? Those are the types of choices facing American families due to the high costs of health care, according to Francois de Brantes, executive director of the Health Care Incentives Improvement Institute (HCI3).. External Link. Opens in new window.
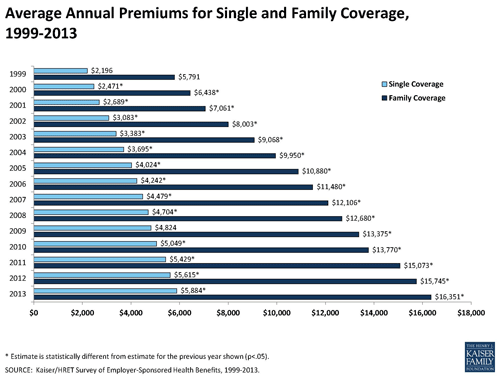
Speaking at The Alliance Annual Meeting on Oct. 22 at The Monona Terrace, de Brantes said 20 percent of the average American household’s income goes to health expenses, including health benefit costs and out-of-pocket expenses.
Different families may make different decisions about what to give up so they can pay for health care, but it’s clear that many families are hurting as a result of making these difficult choices. de Brantes blamed these difficult choices on health care prices that have risen far faster than either wages or other prices.
As a result, de Brantes said health care prices are currently in an inflationary bubble, similar to the bubbles that burst to radically realign the “dot.com” industry and create a meltdown in real estate values. Four factors have contributed to the inflationary bubble, de Brantes said:
- Prices are “opaque,” making it impossible for consumers to shop for health care based on price, or even find out what they”re really paying for.
- Regulatory authorities are either uncaring about this issue or encourage the use of fee-for-service payment models that pay more whenever more health care is provided, even if the additional treatment is due to errors or unnecessary care.
- The health care system fails to pursue payment models that provide incentives for higher efficiency or greater value.
- The burden of paying for health care has been shifted to individuals, who have limited control over health costs or quality despite being required to pay the bill.
As long as health care providers find it easier and more lucrative to raise prices than to improve quality, look for efficiencies and eliminate unnecessary care, de Brantes predicted American families will continue to lose ground.
 “Ultimately, we’re talking about the impoverishment of American families,” de Brantes said. “Is it fair that families have to sacrifice the college educations of their kids so that some in the industry can justify higher prices? We think not.”
“Ultimately, we’re talking about the impoverishment of American families,” de Brantes said. “Is it fair that families have to sacrifice the college educations of their kids so that some in the industry can justify higher prices? We think not.”
de Brantes challenged employers to come together to change the incentives for American health care. Many employers who are members of The Alliance – a cooperative of employers who self-fund their health benefits – have already accepted that challenge by pledging to support the QualityPath™ initiative. QualityPath will identify physicians and hospitals that – when working together – meet proven standards for delivering high-quality, fairly priced care for selected procedures.
Employers who participate in QualityPath will design health benefits that encourage employees to choose high-quality, lower-cost health care providers. Employers and employees alike should know what their cost for the procedure will be when they select a QualityPath provider. That will give families both a better deal and better health care.
Learn more about the QualityPath initiative and the employers who have already pledged their support. There’s still time to join the effort; employers who are Alliance members are welcome to take the QualityPath pledge.
[box]
Learn More about the High Costs of Health Care
- Payment Reform in Health Care
- Employees Wary of Out-of-Pocket Health Care Costs
- Look Upstream to Change the Cost and Outcomes of Care
- Why Controlling Health Care Costs Starts with Primary Care
[/box]
[starbox]







